|
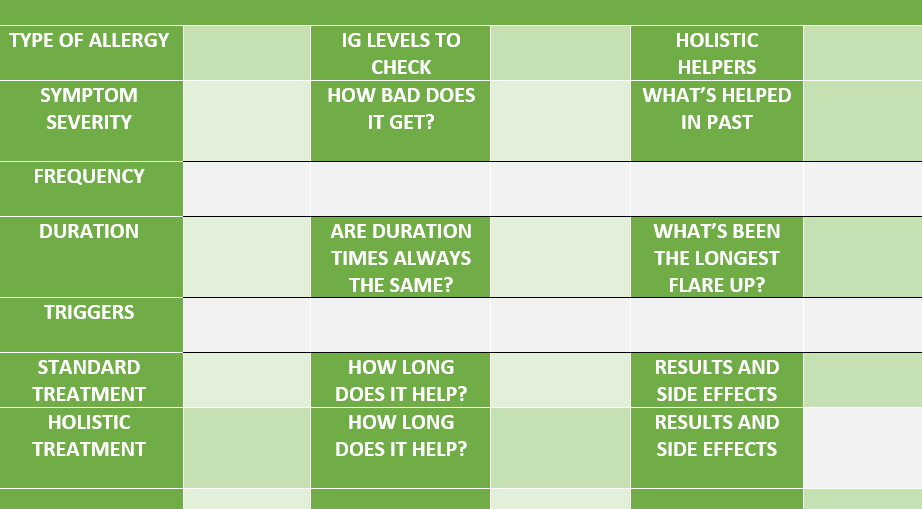
A good mystery throws you right into a story with a lot of characters and clues waiting to be unraveled and explored. Allergies are like that; they're complicated. There's a ton of constantly shifting variables to keep in mind when diagnosing allergies or hypersensitivities. Plus, there are characters like fatigue, weight gain, and muscle pain that could be related to an allergy or possibly other conditions. Once you start investigating it, allergies are more like a maze of confusion than a mystery to solve, so how do we extract what we need from all the information that's been thrown at us? Well, I suppose the first thing we do is gather our facts. Click below to brush up on your allergy knowledge before proceeding. 1. What Are Allergies? Understanding an allergic reaction Learn about common immunoglobins related to allergy The 4 Types of Hypersensitivity 2. Types of Common Allergies 3. How Allergies Are Contracted 4. Symptoms and Triggers Severity, Frequency, Duration Having a fundamental grasp of how allergies work is vital to finding clues inside of facts. While trying to discover what's causing your allergy, lay out all the information in a way that makes sense. Write down your symptoms, how often you get them, their severity, and other details that are pertinent. Compile everything you do know, then fill in the empty spaces as you unwind the mystery. EXAMPLEYou can use a grid like this, or whatever works best for you. Once everything is down in one spot, begin looking for similarities or themes. If you can't solve this one on your own or need further testing, share this grid with your allergist who'll be ecstatic to see you've already done the homework. They'll know the proper next steps to take, and you'll have saved yourself money and time by doing the legwork in advance.
No one expects you to be an expert. That's why doctors specialize in this stuff; it's not easy. But if you don't have access to a doctor or can't afford access to one, this grid can help you find facts, create clues, and hopefully solve the allergy mystery.
0 Comments
Start At The BeginningAn allergic reaction is an overreaction of your immune system, and there are several kinds of hypersensitive responses. Pet, Pollen, Sinus, and Skin allergies are all examples of different types of allergies, and they're also contracted in various ways. Then there are the symptoms. It's like the immune system wanted to make it as complicated as possible to decipher what's going on, but if we can get through other bodily mysteries, by-George, we can solve this one too. Understanding Your SymptomsSymptoms don't necessarily have to line up with the type of allergy you have. You could be suffering from constant congestion due to several different types of allergies (like pet, pollen, or chemical). But even when the allergy type is the same, two people can experience radically different symptoms. Let me give you a better example: If we met the character Pig-Pen from the Peanuts, I'd get a sinus infection, my oldest son would start coughing, my youngest would say his nose hurts, and my husband would have itchy skin. Same stinky character, many different symptoms; same allergen, many different responses, but while knowing your symptoms is important, it doesn't tell us enough. Dr. Leo Galland in his book "The Allergy Solution" presents a unique method to classify symptoms, not just define them. A stuffy nose could mean a million things, so it's wise to classify the symptoms into three categories; severity, frequency, and duration. Dr. Galland suggests monitoring all three as a way to better find what you're allergic to, verses to just responding to the symptoms. How severe is your reaction? How often do you experience your symptoms? How long do they last? Monitor your allergy symptoms like a woman in labor monitors contractions. After tracking your symptoms for a while, you'll undoubtedly have subquestions. The goal is to narrow down your symptoms as much as you can. You may discover that based off of the severity, frequency, and duration of your symptoms, your nose only gets stuffy when you do laundry. Monitoring your symptoms through Dr. Galland's method will help you gauge what's triggering your allergies. What Triggers Your Allergies?Several triggers can cause an allergic reaction, and it's essential to know how you contracted the allergen. Remember you can get allergies through the good old-fashioned gene pool or via injection, consumption, inhalation, and skin contact. So, what causes your symptoms? Here are a few starter questions for finding your triggers:
It's helpful to write these out and just stare at them. What similarities are you finding? What connections are you beginning to make? What do all these triggers and symptoms have in common? A person, place, or thing? Wait, those are nouns, not allergens, we're looking for pronouns, the (specific) cause of your symptoms. If you're trying to figure out what allergies you have and how to treat them on your own, or if you're seeking the help of an allergist, describing your symptom severity, frequency, and duration will help unlock what's going on a whole lot faster. Finding out what triggers your allergies can help prevent them. You could uncover that you have congestion at work, but not home. Your bedroom air freshener could be giving you those headaches or your deep love of cheese could be causing that sinus infection. Classify your symptoms and find your triggers, unless of course, you like leaving mysteries unsolved.
What comes to mind when you think of allergies? Do you think of sniffling and sneezing from pollen, or peanuts and penicillin?
Allergies can encompass the entire body and what makes one person sick doesn't bother the other. Why? People can be allergic to anything from apples to zucchini, and their responses can be just as varied, but one thing is for sure, allergies are becoming more common around the globe.
First, let's look at what allergy technically means. The word itself is based from the Greek word "allos" meaning an altered action or reaction and was first used in the early 1900s.
An allergic reaction happens when your immune system gives an amplified response to a trigger, otherwise known as an allergen. For example, if you're allergic to grass pollen that means your immune system is having an exaggerated response to an allergen ( the grass pollen). Getting rid of your symptoms isn't as easy as taking a Claritin. Most people assume their allergies have something to do with their bodies making too much histamine, so they take medications thinking that'll work, but there's a lot more to it than just that. There are different types of allergies, different kinds of hypersensitivities, plus categories of allergens, so you can understand how diagnosing a particular allergy can be quite tricky. What's Happening Inside My Body?
When an allergen enters your body, your immune system is alerted, and there are a few ways your body can respond. There are four categories of hypersensitivity; we define these by the amount and type of antibodies your body produces for the allergen.
Before we get into more detail, let's meet five-year-old Timmy and learn how an allergic reaction starts. The first time the body is exposed to a trigger it usually doesn't show any symptoms. If little Timmy touches poison ivy for the first time and doesn't break out, that doesn't mean he's not allergic to it. Allergic responses almost always happen in the second or third exposure. The first time Timmy came in contact with the poison ivy, his body remembered it and built antibodies just in case those pesky ivy triggers returned. By the second time he's exposed, his body releases those antibodies, and by the third and fourth exposure, Timmy's immune system is in full war mode; to put it more simply this reaction is a learned behavior by the immune system.
Timmy has an allergic reaction to poison ivy because his immune system created antibodies called immunoglobulins. Immunoglobulins are proteins that act like antibodies inside the immune system. There are various kinds of immunoglobulins and doctors typically measure these to diagnosis the allergy.
After the body creates the immunoglobulins, they adhere to the allergens and release mediators, substances released from cells, like histamine to make Timmy itch and swell. In the most common allergy reaction, a Type 1 Allergy Response, the antibody that the body creates is called immunoglobulin E (henceforth referred to as IgE). The IgE antibodies attach themselves to the allergen then releases what I like to think of as toxic gas, but they're called mediators (like histamine), into the tissues with a bang. Several types of immunoglobulins produce responses inside the body, but IgE is the most common. Timmy's infected arm is red, and he can't stop itching it, so his mother decides it's time to visit the doctor. Getting Diagnosed
Timmy's mom sits next to him in the allergist's office while the doctor performs a "scratch test" on her son.
Skin tests like this are looking for swelling or redness created by the IgE antibodies when they come in contact with various allergens.
Blood tests to determine allergy look for the presence of IgE antibodies in the bloodstream. But allergies go beyond just the antibody IgE. Several other immunoglobins cause responses in your body that your doctor doesn't always look for. Dr. Devi Numburipad writes in his book "Say Goodbye to Illness," "The activation of immunoglobulin type E (IgE) antibodies causes what the traditional medical profession calls 'true' allergies; however, millions of people experience various allergic symptoms every day in varying degrees without producing these antibodies. These types of reactions can be called either intolerance or hypersensitivity."
Here's a breakdown of a few critical immunoglobulins:
IgM is the first antibody released in an allergic reaction (think first responders) IgE is the most common antibody released in allergic response (think itching) IgG is the primary antibody in the blood protecting us against bacteria and viruses. It also creates a delayed allergic reaction from a few hours to even days. (think Lyme's after a tick bite) IgA These antibodies are formed when allergies are related to the mucous membranes. (think congestion)
Putting that information into allergy terms, IgE and IgM antibodies are responsible for the immediate reactions and hypersensitivity to a particular trigger. IgA is the antibody associated with mucus. IgG produces a delayed response to an allergen from hours to even days later. Some people only have IgE antibodies in their bloodstream, but most have more than that, giving us a far better picture of what's going on.
If you have an allergic reaction, your doctor will more than likely perform a scratch test to look for the IgE antibodies, just like little Timmy. But if you're experiencing symptoms related to Lyme's, your doctor will take a blood test and search for the IgG and IgM antibodies. If you're only looking for IgE antibodies, you may be missing something. But just like there are many immunoglobulins and mediators your immune system produces, there are several types of hypersensitivity. While we're waiting on Timmy's scratch test results, let's learn about the different types of hypersensitivity with allergies. TYPES OF HYPERSENSITIVITY RESPONSES
TYPE 1 SENSITIVITY
Type 1 Allergy is the most common and includes asthma, eczema, hives, hay fever, and conjunctivitis. "In type 1 hypersensitivity, B-cells are stimulated (by CD4+TH2 cells) to produce IgE antibodies specific to an antigen. The difference between a normal infectious, immune response and a type 1 hypersensitivity response is that in type 1 hypersensitivity, the antibody is IgE instead of IgA, IgG, or IgM" via Wikipedia. TYPE 2 and 3 HYPERSENSITIVITY Type 2 and 3 are harder to diagnose because standard allergy tests are only looking for IgE. Allergy Types 2 and 3 are dependant on the impact of IgG-the antibody responsible for protecting us against viruses and bacteria- to amplify an allergic response. These types of allergies also produce the symptoms I see most often: food allergies, stomach pain, headaches, fatigue, and joint pain. In Type 3 hypersensitivities, people experience reactions not just from outside forces, but from within their own bodies. IgG is a crucial antibody we need for a healthy immune response. A lack of enough IgG antibodies means you're more likely to suffer from recurring bacterial infections big or small, and people with autoimmune disease often have lower amounts of IgG antibodies circulating in their bloodstream and fewer T-reg cells, making for a weaker immune system. TYPE 4 HYPERSENSITIVITY Type 4 Hypersensitivity skips the entire "create antibodies, release mediators, and inflame" part and goes right into killer immune system mode, like a Code Red at the Pentagon, but there's a delayed response. Poison ivy and oak are both examples of Type 4 Hypersensitivity because of the delayed response. In this type of reaction, the immune system bypasses creating antibodies and calls in the big guns named Helper Lymphocytes. Lymphocytes are white cells made to protect the body from disease and include B cells and T cells. The Helpers then recruit the Killer Lymphocytes. The Killers go right to the allergen and destroy, destroy, destroy. Sounds great until you realize that the Helper and Killer cells also produce mediators while they combat the allergen. Helper Lymphocytes are even involved in the damage that happens in RA, Crohn's disease, Hashimoto's, and other autoimmune diseases.
Allergy responses fluctuate and very rarely does anyone only have one reaction and one type of allergy, most often it's a mixture of many factors.
The allergist returns and writes in her patient file "IgE positive, moderate response/Type 4" then looks up to Timmy's mom. "Well, it looks like he's just reacting to poison ivy and symptoms should get better in a few days- no scratching- call me if you need anything else." and she slips out of the room. Timmy's case was pretty open and shut, but many allergies don't just affect your nose or your skin. Weight gain, fatigue, bloating, brain fog, headaches, constipation, and joint pain are all symptoms of allergic reactions. "Allergy occurs when the part of your immune system that controls unwanted immune responses fails to function properly. It's actually an immune deficiency state that results in excessive inflammation." says Dr. Leo Galland in his book "The Allergy Solution." Some allergies you can control, others reverse, and many you can prevent. But before you know how to fight back, you must first understand what you're working with, and it's not histamine, it's your immune system.
Numerous studies have proven that a stable and functioning immune system is essential for ridding yourself of allergy symptoms. The way we develop that strength is by eating a whole food diet with particular attention paid to foods that will support your immune system with the best flavonoids and phytonutrients.
If you're suffering frequent headaches, sinus infections, or fatigue there's a chance it's coming from an allergy. Understanding what your body is doing is essential before you pop that pill or walk into the doctor's office. Educate yourself and make sure you're being tested for the right antibodies and are receiving the proper treatment for your symptoms. Once you know the details, you can create a plan to prevent, control, and maybe even heal your allergies. |
Categories
All
Linda's BlogsArchives
October 2019
AuthorLinda Lavender writes articles to help folks with Auto Immune Disease, Depression, Anxiety and other health related illnesses. |




 RSS Feed
RSS Feed